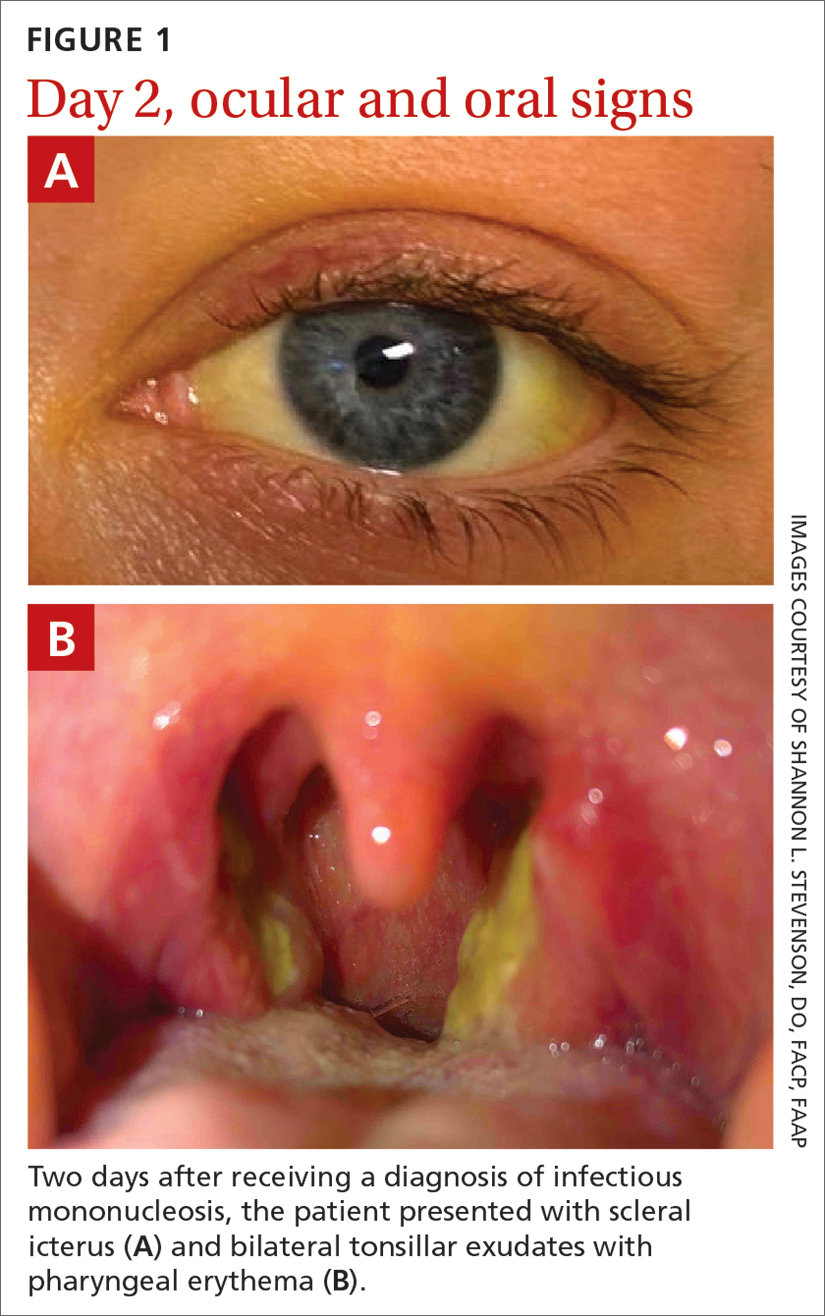
Prolonged hemolysis can lead to severe unconjugated hyperbilirubinemia in patients with concurrent hepatic dysfunction. 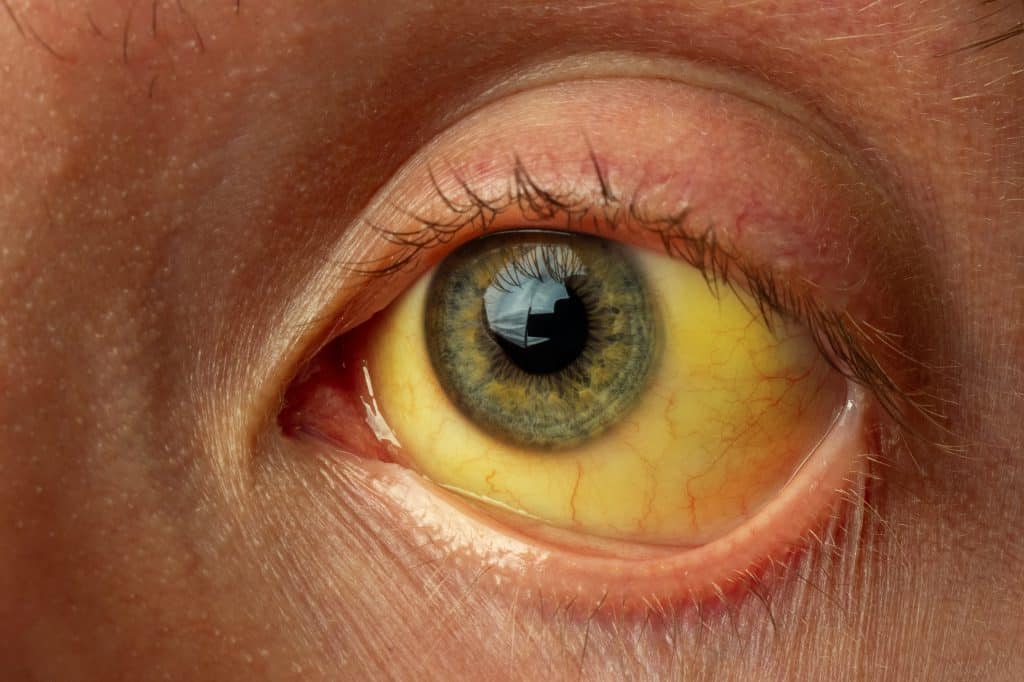
As a result, the serum levels of unconjugated bilirubin remain modest (1 to 4 mg/dL) and rarely exceed 4 mg/dL. In these conditions, patients with normal liver function efficiently conjugate and excrete the excess bilirubin. 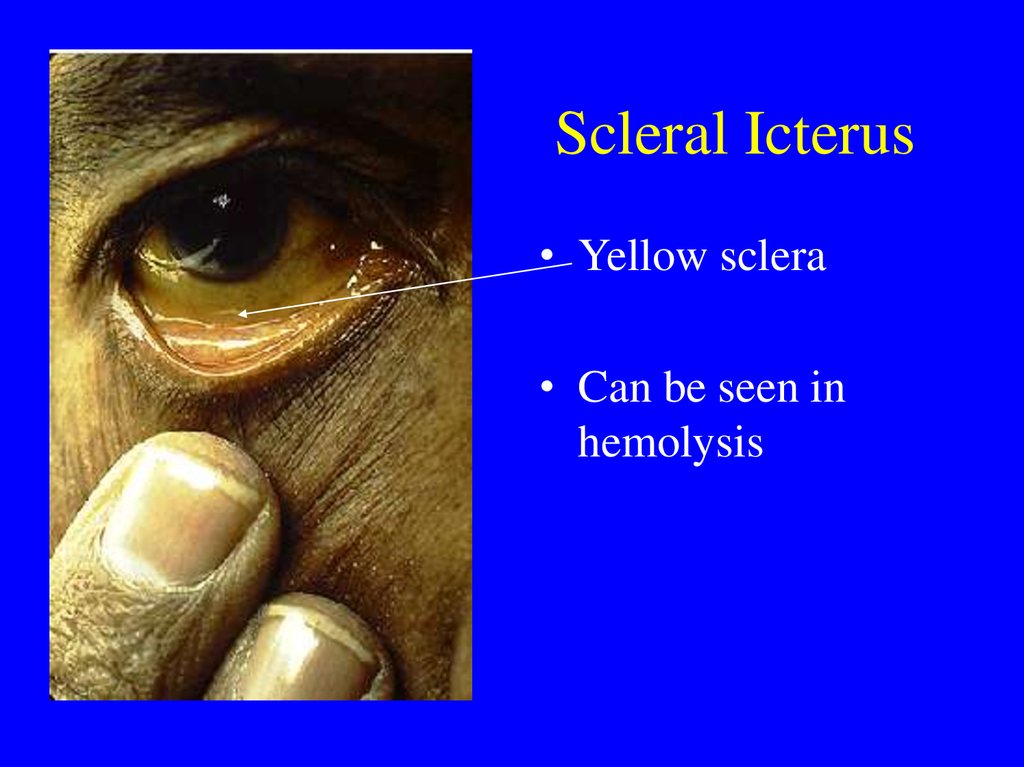
Increased bilirubin production and consequential unconjugated hyperbilirubinemia can result from increased catabolic degradation of hemoglobin and other heme proteins, typically due to accelerated hemolysis, a large hematoma, dyserythropoiesis (e.g., megaloblastic and sideroblastic anemias), or sometimes due to destruction of transfused erythrocytes. Unconjugated hyperbilirubinemia arises in one of the three major pathophysiologic conditions or a combination of them: In neonates, inefficient conjugation of bilirubin leads to unconjugated hyperbilirubinemia (physiologic neonatal jaundice). Therefore, unconjugated hyperbilirubinemia can result from dysfunction of any of these conjugation steps. This process also reduces the ability of bilirubin to diffuse across the blood-brain barrier. The conjugated bilirubin (CB) is then pumped into bile via an energy-requiring process requiring the multidrug resistance-associated protein 2 (MRP2). Conjugation increases the solubility of bilirubin in plasma and thereby enhances its elimination from the body. Next, unconjugated bilirubin gets conjugated with one or two molecules of glucuronic acid by the enzyme uridine diphospho-glucuronate glucuronosyltransferase (UGT1A1), which forms bilirubin monoglucuronide and bilirubin diglucuronide respectively. In liver hepatocytes, UCB dissociates from albumin and binds to proteins of the glutathione-S-transferases family that present it for conjugation and prevent it from effluxing from the liver. The entry of UCB into the liver has not been elucidated, and the best candidate appears to be a bilirubin transporter. UCB tightly bound to albumin is transported to the liver. 
The conversion of heme to bilirubin is a two-step reaction, in the first step the microsomal heme oxygenase enzyme of the reticuloendothelial system, converts heme to biliverdin, which in turn is reduced to unconjugated bilirubin (UCB) by a second enzyme biliverdin reductase. Approximately 85 percent of the heme moiety comes from the hemoglobin degradation of red blood cells, while the remaining derives from the ineffective erythropoiesis and the breakdown of other hemoproteins such as cytochromes, myoglobin, and catalase. īilirubin, a yellow-orange bile pigment, is the catabolic product of heme metabolism. Several inherited disorders can also produce unconjugated hyperbilirubinemia, including Gilbert syndrome, Crigler-Najjar syndromes type I and II, and inherited disorders causing hemolytic anemia. In newborns, the increased concentration of UCB can cross the blood-brain barrier, and deposit in the basal ganglia or cerebellum causing a bilirubin-induced encephalopathy or kernicterus. In neonates, jaundice typically occurs due to unconjugated hyperbilirubinemia, which is characterized by the increased levels of indirect or unconjugated bilirubin (UCB) in the serum. Unconjugated hyperbilirubinemia (albumin-bound) usually results from increased production, impaired hepatic uptake, and decreased conjugation of bilirubin. Depending on the form of bilirubin present in serum, hyperbilirubinemia can be further classified as unconjugated (indirect) or conjugated (direct). Hyperbilirubinemia is a condition defined as elevated serum or plasma bilirubin levels above the reference range of the laboratory, and it is due to disorders of bilirubin metabolism.
0 Comments
Leave a Reply. |
Details
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
